Research Outlook with Prof Gareth Evans
09 April 2019
Research Outlook with Prof Gareth Evans
Prof Gareth Evans is the Chair of the Medical Advisory Board of Nerve Tumours UK, and has an established international reputation in the treatment and research of Neurofibromatosis. Here he gives a brief overview of the current research landscape for NF.
There is very little funded research in the UK – the research in the UK which is published is rarely fully funded. We are reliant for the most part on developments in the US, which is underpinned by around $15m a year in grants from the US Department of Defense.
The most hopeful developments are in drug treatments, MEK Inhibitors for NF1, and Avastin for NF2 (each described below). I am hopeful that these drug treatments will become mainstays in UK treatment.
NF2: Avastin
Extract from Addenbrooke’s Hospital, Cambridge:
Avastin is a type of drug treatment known as antiangiogenic therapy. It works by blocking signals made by tumours that cause blood vessels to grow in their vicinity. Without the
support of blood vessels, the tumour lacks nutrients and oxygen needed to grow. The NHS national programme for Avastin therapy for NF2 patients has been running since 2010. The
latest evaluation shows that in 90% of patients the tumour either shrinks or stops growing and hearing function either stabilises or improves in 86% of patients.
Extract from Oxford University Hospitals’ information guide:
Avastin is given to people with NF2 when a schwannoma has grown by a specific amount or more over the previous year. The schwannoma will be measured by looking at and comparing
MRI scans over the course of a year. Evidence suggests that Avastin is more effective in faster growing tumours. National guidelines state that patients need to have schwannomas that meet the specific growth rate criteria for them to be considered for treatment with Avastin.
Avastin is given for the treatment of NF2 initially for six months, with three monthly MRI scans and clinic reviews. If a tumour starts to grow despite having Avastin treatment, then the drug will be stopped. The drug will also be stopped if you suffer significant side effects.
– Prof Gareth Evans"The latest evaluation shows that in 90% of patients the tumour either shrinks or stops growing"
NF1: MEK Inhibitors
Neurofibromin is the protein which is downstream of the NF1 gene, and suppresses the proliferation of
tumours. It is its absence that causes tumours for people with NF1. The way that MEK Inhibitors work has been helpfully described by Dr Annette Bakker, President and Chief Scientific Officer of the Children’s Tumor Foundation, in the US. She uses the analogy of an unruly classroom, where neurofibromin is the teacher who normally keeps control, but is absent. MEK is the naughtiest child in the class, who causes most of the trouble in the absence of the teacher. The MEK Inhibitor drug keeps that naughty child under control.
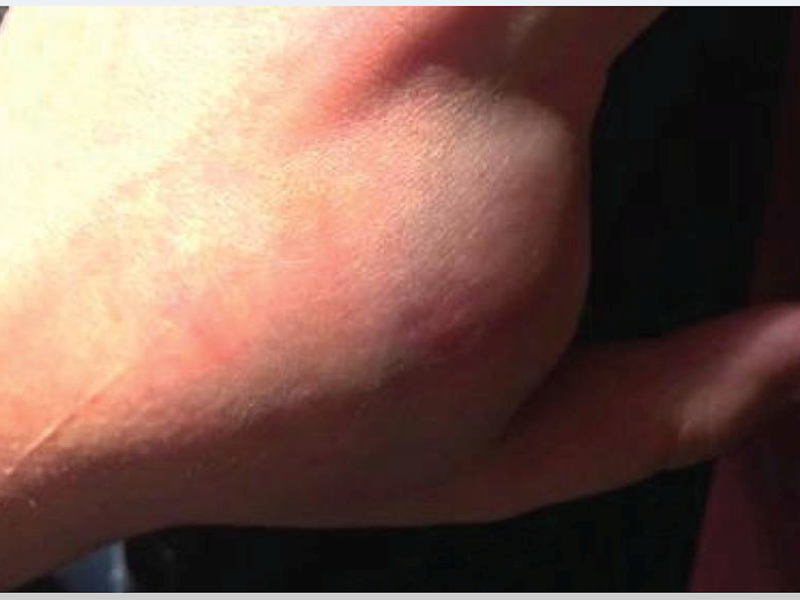
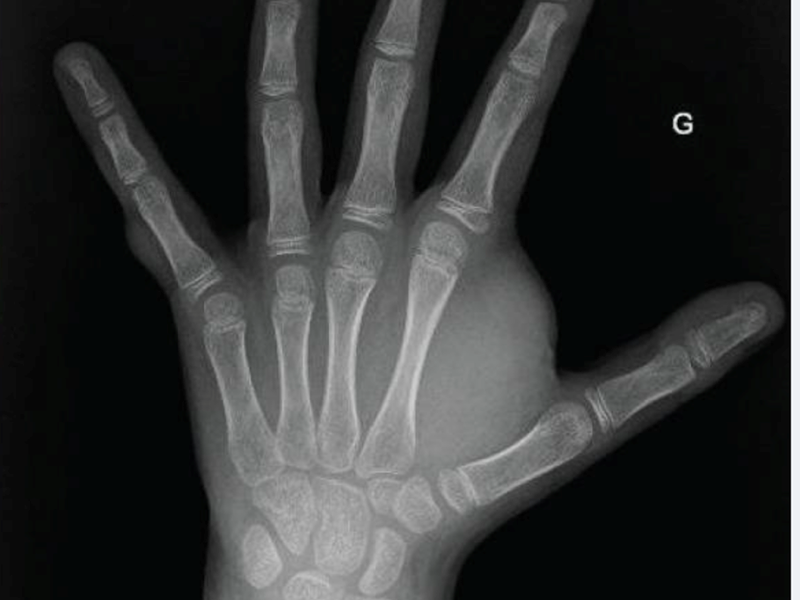
Subcutaneous neurofibroma (left hand): X-ray and photograph
A study by French researchers reported in ecancermedicalscience, showed dramatic results in a 12-year-old boy with NF1, who was finding walking impossible, and suffering increased pain in his hand (see images on the right). Within a week of beginning treatment with a MEK Inhibitor, Trametinib, he was walking again, and the pain had disappeared. These results were sustained, and after a year, he no longer needed to take the drug.
MEK Inhibitors are currently undergoing clinical trials in the US, and are showing similarly ‘spectacular’ results. The Children’s Tumor Foundation are hopeful they will soon be approved
for patient treatment.
– Prof Gareth Evans"Within a week of beginning treatment with a MEK Inhibitor, Trametinib, he was walking again, and the pain had disappeared."
Filter News

Fyling Fest Fundraiser
Fyling Fest 2025: Sunshine, music & a whole lot of heart in the Rose Garden - all in support of Bea
Read More
Bea’s Story: Courage and Resilience
Bea, 'Bringer of Joy', never stops smiling despite her condition & NF1 related complications - read her story
Read More
Margaret’s Story
Margaret reflects on life with NF and her involvement with the charity since its early days
Read More
Repurposing anti-retroviral drugs to treat NF2 related tumours Retreat Study
Join a brand new study treating tumours in NF2 patients.
Read More
Raising Awareness: Georgia’s Blog
My name is Georgia Baum, I’m 25 years old and an Ambassador for Nerve Tumours UK. Read my Blog and follow my journey!
Read More
Be Kind and Be Brave
December Coffee Club at Guy's and St Thomas' - A Christmas Karma Special Screening
Read More
Christmas Message from the NTUK Head Office Team
Happy Christmas from all of us at Nerve Tumours UK
Read More
Oliver Bromley - Reflections of 2025 - Outlook to 2026
“Looking back, looking forward – A year in the life of the NF community”
Read More


